What Is Tooth Remineralization and How Does It Work?
Your teeth are under attack every single day — and most people have no idea it is happening. Every sip of coffee, every bite of bread, and every meal you eat triggers a microscopic battle on the surface of your enamel. The good news is that your body has a built-in defense system that fights back. That process is called tooth remineralization, and understanding it could be the single most important thing you do for your long-term dental health.
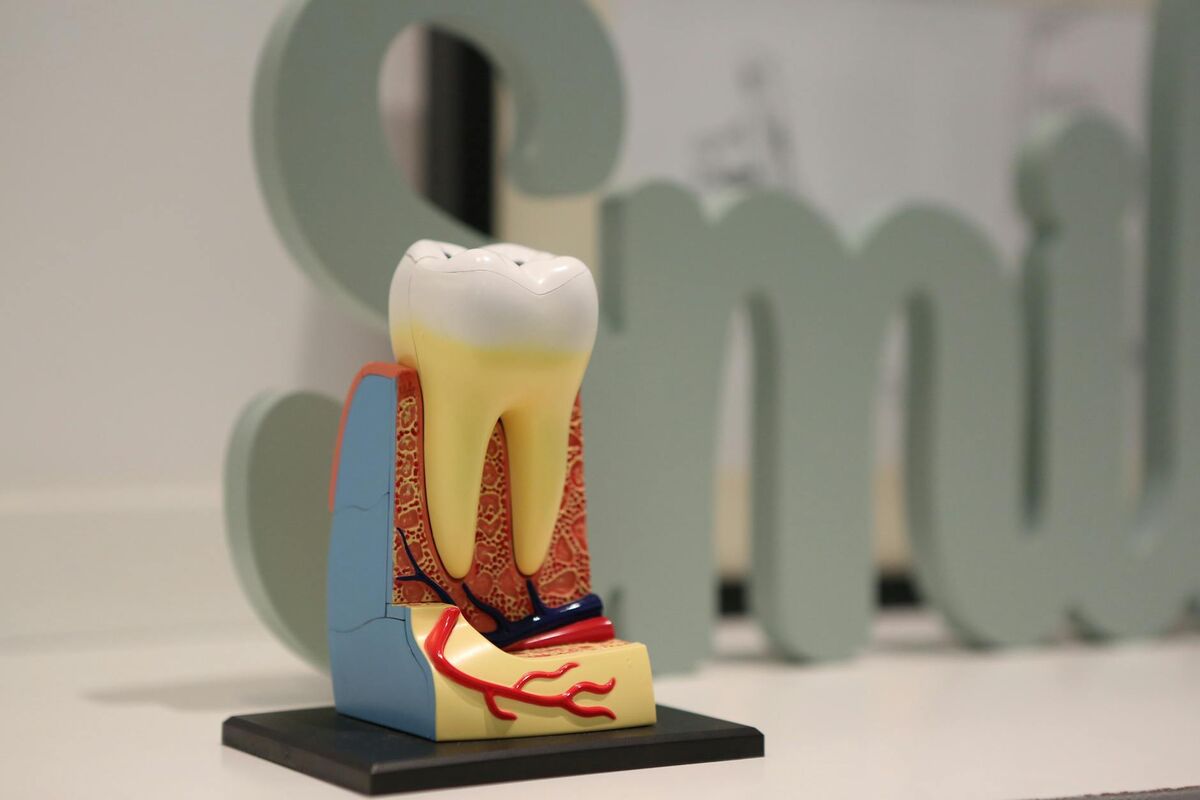
Tooth enamel is the hardest substance your body produces — harder than bone. It is the thin but extraordinarily tough outer shell covering each tooth, and it serves as the first and only line of defense against the acids, bacteria, and physical forces your mouth encounters daily. Yet despite its strength, enamel is vulnerable to one thing above all others: acid.
One of the most persistent myths in dental health is that enamel, once damaged, is gone forever. While it is true that enamel cannot regenerate the way skin or bone can — because it contains no living cells once the tooth has erupted — this does not mean early-stage enamel damage is irreversible. Tooth remineralization is the natural process through which minerals are redeposited into partially demineralized enamel, effectively repairing microscopic damage before it becomes a cavity. The distinction matters enormously: you cannot grow back enamel that has been completely eroded, but you absolutely can reverse early mineral loss and strengthen weakened enamel before it reaches that point.
This guide explains the science behind demineralization and remineralization, why modern diets are tipping the balance toward decay, and what evidence-based strategies can help you shift that balance back in your favor.
Understanding Demineralization: What Happens Every Time You Eat
To understand tooth remineralization, you first need to understand what it is reversing. Demineralization is the process by which acid dissolves the mineral content of tooth enamel. The primary mineral involved is hydroxyapatite, a crystalline calcium phosphate compound that gives enamel its remarkable hardness. When acid contacts the tooth surface, it disrupts the crystal lattice of hydroxyapatite, leaching calcium and phosphate ions out of the enamel and into the surrounding saliva.
There are two main sources of this acid. The first is dietary acid — found in citrus fruits, vinegar, carbonated drinks (including sparkling water), wine, and many fermented foods. The second, and far more damaging over time, is bacterial acid. The oral microbiome contains hundreds of bacterial species. When certain bacteria — particularly Streptococcus mutans — metabolize fermentable carbohydrates (sugars and refined starches), they produce lactic acid as a byproduct. This acid pools in the plaque biofilm sitting directly against the tooth surface, creating a localized acidic environment that drives demineralization far more efficiently than dietary acid alone.
The critical threshold is a pH of approximately 5.5. At or below this level — known as the critical pH for enamel dissolution — demineralization outpaces remineralization. Studies using quantitative light-induced fluorescence have shown that after a single sugar exposure, plaque pH can drop below 5.5 within two to five minutes and remain there for up to 40 minutes. Each meal or sugary snack therefore represents a fresh 40-minute window during which your enamel is losing mineral content.
Early demineralization is not visible to the naked eye. The first clinical sign is a white spot lesion — a chalky, opaque patch on the enamel surface caused by changes in how the mineral-depleted enamel scatters light. This is the stage at which remineralization can still reverse the damage. Once the lesion progresses through the enamel into the dentine beneath, a physical cavity has formed and only a dentist can repair it. This progression from white spot to cavity can take months or even years in adults, which is exactly why the remineralization window is so valuable.

The Remineralization Process: How Your Body Fights Back
The most powerful remineralization tool you have is also the one you take most for granted: your saliva. Saliva is not simply a lubricant — it is a sophisticated biological fluid specifically engineered to protect and repair your teeth. Understanding how it works explains a great deal about why some people are far more cavity-prone than others.
Saliva performs remineralization in several distinct ways. First, it acts as a pH buffer. Bicarbonate and phosphate ions in saliva neutralize acid in the mouth after eating, raising plaque pH back above the critical 5.5 threshold. The faster your saliva neutralizes this acid, the less time enamel spends in a demineralizing environment. Second, saliva is supersaturated with calcium and phosphate ions relative to the concentrations found in enamel. This concentration gradient drives the passive diffusion of these minerals back into the demineralized enamel crystal lattice — essentially refilling the gaps left by acid dissolution.
The specific minerals involved in remineralization are:
- Calcium (Ca²⁺) — the primary structural cation in hydroxyapatite, essential for rebuilding the enamel crystal.
- Phosphate (PO₄³⁻) — combines with calcium to reform hydroxyapatite; saliva is the primary source during natural remineralization.
- Fluoride (F⁻) — does not rebuild enamel in the conventional sense but catalyzes the process dramatically. Fluoride substitutes for hydroxyl groups in the hydroxyapatite crystal, producing fluorapatite, which is significantly more resistant to acid dissolution than the original mineral. Even at very low concentrations (around 1 ppm), fluoride in saliva accelerates remineralization and lowers the critical pH threshold from 5.5 to approximately 4.5.
- Nano hydroxyapatite (nHAp) — a synthetic form of the mineral that directly integrates into the enamel structure. A growing body of research, including a 2019 systematic review published in the British Dental Journal, has found nano hydroxyapatite to be comparable to fluoride in remineralizing early enamel lesions.
The daily cycle of mineral exchange in your mouth is sometimes called the demineralization-remineralization equilibrium. Think of it like a savings account: every meal makes a withdrawal (demineralization), and the rest of the day — when your saliva has time to work — makes deposits (remineralization). In a healthy mouth with a balanced diet and good saliva flow, deposits consistently exceed withdrawals and teeth remain strong. In a mouth with frequent sugar exposure, poor saliva flow, or chronically low pH, withdrawals outpace deposits and enamel gradually weakens.
Why do some people remineralize better? Saliva flow rate is the biggest individual variable. People who produce more saliva — or whose saliva has higher buffering capacity — remineralize faster. Genetic factors influence both saliva composition and enamel crystal structure. Age also plays a role: saliva production tends to decline after age 50, and many medications commonly taken by older adults (antihistamines, antidepressants, blood pressure drugs) cause xerostomia (dry mouth), significantly impairing remineralization capacity.
Natural Ways to Enhance Tooth Remineralization
The most effective way to support tooth remineralization is to shift the daily mineral balance in your favor through consistent, evidence-based habits. None of these require expensive products — most are dietary and behavioral changes that cost nothing.
1. Increase Calcium and Phosphate Through Diet
The minerals needed for remineralization must come from somewhere, and diet is their primary source. Foods rich in calcium and phosphate directly increase the concentration of these ions in saliva. Dairy products — particularly hard cheeses — are exceptionally useful because they not only deliver calcium and phosphate but also stimulate saliva flow and raise plaque pH. A 2015 study published in the Journal of the American Dental Association found that eating cheese after a sugary food significantly neutralized the acid challenge compared to eating the same food without cheese. Other excellent dietary sources include leafy greens (kale, bok choy), canned fish with soft bones, almonds, tofu, and legumes.

2. Manage Acid Exposure — Timing Matters as Much as Quantity
Reducing acid exposure is not just about eating fewer acidic foods — it is about the pattern of exposure. Sipping a glass of orange juice over two hours exposes your enamel to acid continuously for that entire period, never allowing plaque pH to recover. Drinking the same juice in five minutes creates a single 40-minute acid challenge. Research consistently shows that frequency of sugar and acid exposure is a stronger predictor of tooth decay than total quantity consumed. Condensing acidic or sugary foods to mealtimes, rather than grazing throughout the day, can dramatically reduce cumulative acid attack time.
Rinsing with plain water immediately after eating acidic foods helps dilute and clear acid from the mouth. However, brushing immediately after acidic food or drink is counterproductive — enamel is softened in the first 30 minutes after acid exposure, and brushing during this window can physically remove weakened enamel. Wait at least 30 to 60 minutes before brushing.
3. Stimulate Saliva Production
Since saliva is the primary vehicle for natural tooth remineralization, increasing salivary flow is one of the highest-leverage interventions available. Sugar-free gum — particularly gum sweetened with xylitol — is the most evidence-backed saliva stimulant. Chewing for 20 minutes after meals has been shown to raise plaque pH, increase saliva flow, and deliver additional calcium and phosphate to the tooth surface. Staying well hydrated also supports adequate saliva production; chronic mild dehydration is a common and overlooked cause of reduced saliva flow.
4. Use Xylitol and Erythritol Strategically
Xylitol is a sugar alcohol that cannot be fermented by Streptococcus mutans. Regular consumption — ideally 5–10 grams per day spread across several exposures — has been shown in multiple randomized controlled trials to reduce S. mutans counts in plaque, lower the rate of bacterial acid production, and support remineralization by keeping plaque pH elevated. Erythritol has shown similar and in some studies superior antibacterial properties. Replacing regular mints, gum, and sweets with xylitol or erythritol versions is a simple, sustainable way to reduce the acid burden on your teeth throughout the day.
5. Do Not Neglect Vitamin D
Vitamin D is required for the intestinal absorption of calcium. Without adequate vitamin D, dietary calcium intake has limited benefit for tooth remineralization because much of it is never absorbed into the bloodstream and therefore never reaches the saliva. A 2013 meta-analysis in Nutrition Reviews found that vitamin D supplementation reduced caries risk by approximately 47% in children — a striking effect size driven largely by improved calcium metabolism. Adults with low sun exposure should consider having their serum vitamin D levels checked.
Products That Support Remineralization
Beyond dietary strategies, several categories of dental products have solid evidence behind them for enhancing tooth enamel repair and supporting the remineralization process.
Fluoride Toothpaste
Fluoride remains the most extensively studied and proven remineralization agent available. It works by incorporating into the enamel crystal as fluorapatite, which is more resistant to acid than the original mineral. Standard toothpaste contains 1,000–1,500 ppm fluoride — sufficient for adults with normal decay risk. High-fluoride prescription toothpastes (5,000 ppm) are available for people at elevated risk and have demonstrated significantly faster remineralization of white spot lesions in clinical trials. The key is to spit rather than rinse after brushing, leaving a fluoride film on the teeth to continue working overnight.
Nano Hydroxyapatite Toothpaste
Nano hydroxyapatite toothpaste has emerged as a credible fluoride alternative — particularly relevant for parents of young children, pregnant women, and individuals who prefer fluoride-free options. Because nano hydroxyapatite particles are chemically identical to the mineral already in enamel, they integrate directly into the enamel surface and fill submicron defects. A 2020 clinical trial in the Journal of Dentistry found that a nano hydroxyapatite toothpaste performed equivalently to a 1,450 ppm fluoride toothpaste in remineralizing artificial white spot lesions over a four-week period.
Calcium Phosphate Products (ACP and CPP-ACP)
Amorphous calcium phosphate (ACP) and casein phosphopeptide-stabilized ACP (CPP-ACP) are available in dental creams and chewing gums. CPP-ACP works by keeping calcium and phosphate in an amorphous (non-crystalline) state near the tooth surface, available for rapid remineralization when pH drops. Multiple clinical studies have found CPP-ACP products to be effective at reversing white spot lesions, particularly when used in combination with fluoride.
Remineralizing Mouthwashes
Fluoride mouthwashes used after brushing provide an additional fluoride dose and extend contact time between fluoride and the enamel surface. Alcohol-free formulations are preferred because alcohol can dry out oral tissues and reduce saliva production — the opposite of what you want for tooth remineralization. Mouthwashes containing xylitol add an antibacterial component to the mineral delivery.
When to See a Dentist: Signs Remineralization Is Not Enough
Understanding the limits of tooth remineralization is just as important as knowing its possibilities. Remineralization is a surface-level process — it can repair early enamel lesions where the outer surface is still structurally intact (even if mineral-depleted), but it cannot rebuild enamel that has physically cavitated or been lost through erosion.
You should see a dentist if you notice any of the following:
- Visible pitting or holes in tooth surfaces — these represent physical cavities that require restoration
- Persistent tooth sensitivity to cold, heat, or sweetness that lasts more than a few seconds — this suggests dentinal involvement, meaning enamel loss has exposed the porous layer beneath
- White spot lesions that are not improving after 3–6 months of consistent remineralizing home care
- Visible darkening inside a white spot — a sign of active caries progression
- Generalized enamel thinning or translucency at the edges of the front teeth, particularly in people with acid reflux, frequent vomiting, or who consume large amounts of acidic beverages
- Chronic dry mouth that does not respond to hydration strategies — your dentist may prescribe high-fluoride toothpaste or other prescription-strength remineralizing agents
Professional treatments available through a dentist include fluoride varnish applications (which deliver fluoride at concentrations 100 times higher than toothpaste), silver diamine fluoride (SDF) for arresting active lesions, resin infiltration (a micro-invasive technique that seals white spot lesions with a resin that matches enamel's refractive index), and for more advanced damage, composite bonding or porcelain restorations.
It is also worth emphasizing that tooth remineralization strategies work best as prevention and early intervention — not as a substitute for regular dental check-ups. A dentist can identify demineralization at stages invisible to you, assess your individual risk factors, and tailor a remineralization protocol to your specific needs.
Key Takeaways
Tooth remineralization is one of the most underappreciated processes in human biology. Your teeth are not static — they are engaged in a continuous, dynamic exchange of minerals with the saliva around them. Every day, enamel loses minerals to acid and regains them through the action of saliva. When that balance is maintained or tipped toward remineralization, teeth remain strong and decay is prevented. When it tips toward demineralization — through frequent sugar exposure, poor saliva flow, or nutritional deficiencies — enamel gradually weakens and cavities eventually form.
The practical implications are clear. Reducing the frequency of acidic and sugary food exposure, eating a mineral-rich diet, staying hydrated, using fluoride or nano hydroxyapatite toothpaste correctly, and incorporating xylitol into your daily routine are all evidence-backed ways to support how to remineralize teeth naturally and enhance your body's innate repair capacity. These are not exotic interventions — they are accessible, low-cost habits that compound over time into dramatically better dental outcomes.
The answer to the question "can tooth enamel grow back?" is nuanced: lost enamel cannot regenerate, but early mineral loss absolutely can be reversed through consistent remineralization strategies. The earlier you intervene, the more you preserve. And preserving your enamel today is always better than restoring a cavity tomorrow.
Summary: Key Points on Tooth Remineralization
- Enamel undergoes a daily cycle of mineral loss (demineralization) and mineral gain (remineralization)
- Acid from bacteria and diet drives demineralization — frequency of exposure matters more than quantity
- Saliva is the primary vehicle for natural remineralization, delivering calcium, phosphate, and fluoride
- White spot lesions are reversible; physical cavities are not — catching damage early is critical
- Calcium-rich foods, xylitol gum, fluoride or nano hydroxyapatite toothpaste, and vitamin D all support remineralization
- Brush 30–60 minutes after acidic foods; spit but do not rinse after brushing to maximize fluoride contact time
- Persistent sensitivity, visible pitting, or non-improving white spots require professional dental evaluation