10 Early Warning Signs of Tooth Decay You Shouldn't Ignore
Something feels off. Maybe your tooth winces when you sip cold water. Maybe you noticed a dull ache that wasn't there last month, or a small dark spot that you keep hoping is just a shadow. Your instinct is telling you something — and that instinct is worth listening to.
The early signs of tooth decay are often subtle, easy to dismiss, and incredibly important not to ignore. Tooth decay is the most common chronic disease in the world, yet it doesn't happen overnight. It progresses through distinct stages, and at several of those stages — particularly the earliest ones — it is completely reversible or highly treatable with minimal intervention.
The problem is that most people wait until something hurts before they act. By then, a cavity warning sign that could have been handled with a fluoride treatment or a small filling may have become a root canal or an extraction. This guide walks you through all 10 warning signs in order of progression, explains the biology behind each one, and tells you exactly what you can do about it at every stage.
Understanding How Tooth Decay Progresses
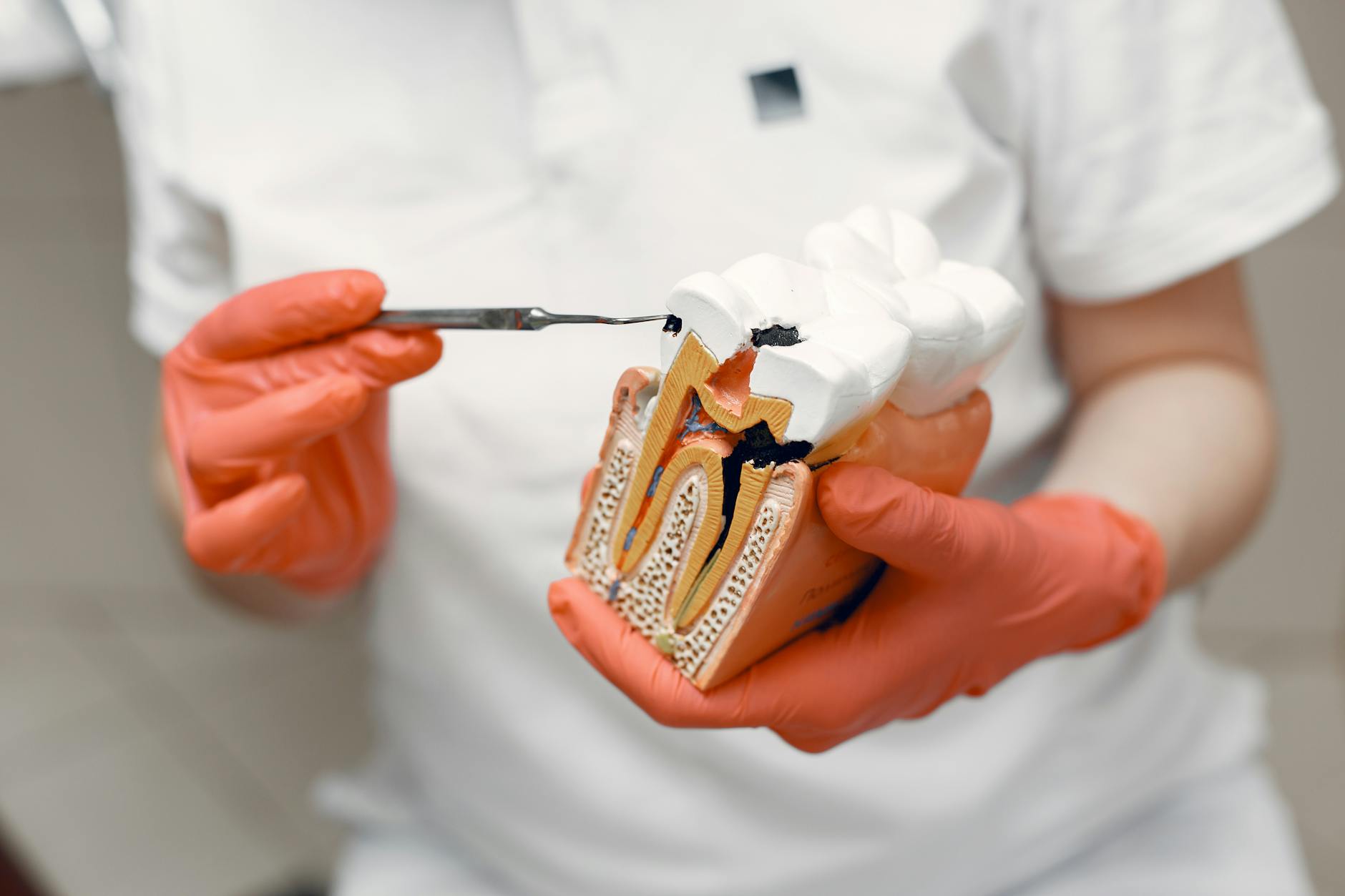
Before diving into the specific cavity warning signs, it helps to understand what's actually happening inside your tooth. Decay doesn't start as a hole — it starts as a chemical process.
The bacteria naturally present in your mouth feed on sugars and starches from your diet. As they metabolize these foods, they produce acids. Those acids attack the outer surface of your teeth — the enamel — in a process called demineralization. Your saliva works to counteract this by delivering calcium and phosphate back to the enamel, a process called remineralization. When acid attacks outpace the body's ability to remineralize, decay begins to take hold.
The progression of tooth decay stages follows a predictable path:
- Stage 1 — Initial demineralization: Subsurface mineral loss; no cavity yet. Fully reversible.
- Stage 2 — Enamel decay: Surface of enamel breaks down. Early cavity. Treatable with small fillings.
- Stage 3 — Dentin decay: Bacteria reach the softer layer beneath enamel. Sensitivity increases sharply.
- Stage 4 — Pulp involvement: Bacteria reach the nerve and blood vessels. Pain becomes significant.
- Stage 5 — Abscess: Infection spreads to surrounding tissue. A dental emergency.
The key takeaway: stages 1 and 2 are where you want to catch this. At stage 1, no drilling is needed at all. At stage 2, a simple filling resolves the problem. Every stage beyond that means more treatment, more time, and more money. Knowing the early signs of tooth decay gives you the power to act before it escalates.
The 10 Early Warning Signs of Tooth Decay
1. White Spots or Chalky Patches on Your Teeth
The very first visible sign of tooth decay is not a hole — it is a white spot. These chalky, opaque patches appear on the surface of the enamel and signal that minerals are being leached from that area. They are most commonly found near the gumline or on the smooth surfaces of the teeth, and they look distinctly different from the natural translucency of healthy enamel.
These white spots represent subsurface demineralization, meaning the structure just beneath the enamel surface has begun to lose calcium and phosphate. The enamel itself has not yet broken down — and this is the crucial detail. At this stage, the process is entirely reversible. Fluoride treatments, remineralizing toothpastes containing hydroxyapatite, and improved oral hygiene can restore mineral density and eliminate the white spot before a cavity ever forms.
Do not confuse these with fluorosis spots (which appear during tooth development) or developmental hypomineralization. If you are unsure, a dentist can distinguish them on sight. The action item here is simple: book a checkup, mention the spots, and ask about remineralization therapy.
2. Tooth Sensitivity to Temperature
If cold water, ice cream, or a hot cup of tea causes a sharp or lingering twinge in a specific tooth, pay attention. Temperature sensitivity is one of the most common cavity warning signs and one of the earliest sensory signals that enamel has been compromised.
Here's the biology: beneath the enamel lies a layer called dentin, which is riddled with tiny tubules that connect to the nerve of the tooth. Healthy enamel insulates these tubules from thermal changes. When enamel thins or a small cavity forms, temperature changes travel through these tubules and stimulate the nerve directly — producing that recognizable zap of sensitivity.
Cold sensitivity tends to appear earlier in tooth decay stages than heat sensitivity. If you experience lingering pain after hot foods or drinks that lasts more than a few seconds, that is a more serious sign that the nerve may be involved. A single, brief twinge from cold is concerning enough to mention to a dentist, but heat sensitivity warrants a more urgent appointment.
3. Sensitivity or Pain When Eating Sweets
Sensitivity specifically triggered by sweet foods — candy, juice, sugary coffee — is another distinct early warning sign worth noting separately from temperature sensitivity. It points to exposed or damaged enamel and early dentin involvement.
The explanation lies in osmotic pressure. Sugars are osmotically active molecules, meaning they draw fluid through those same dentinal tubules when enamel is thin or breached. This fluid movement stimulates the dental nerve, producing pain or discomfort. The fact that it is sweets specifically triggering the sensation — rather than all foods — is diagnostically meaningful. It often indicates early-to-mid stage enamel breakdown rather than advanced pulp involvement.
If your teeth ache after sugary foods, consider it a direct communication from your mouth that the enamel's defenses have been weakened in that area. Cut back on frequency of sugar exposure, increase remineralizing habits, and schedule a dental visit soon.
4. Brown or Gray Discoloration on a Tooth
Once a white spot progresses past the initial demineralization phase and enamel begins to break down further, the area often darkens. You may notice a brown, tan, or gray patch on the tooth surface that wasn't there before. This discoloration reflects deeper mineral loss and the beginning of structural enamel breakdown — a more advanced phase of the early tooth decay stages.
It is important to differentiate decay-related discoloration from surface staining. Staining from coffee, tea, or tobacco tends to be diffuse and located along the gumline or between teeth uniformly. Decay discoloration is more localized — often appearing in the grooves of back teeth or in pits — and may have a slightly soft or matte texture rather than a hard, smooth surface.
At this stage, a cavity likely exists and will need a filling. However, it is still a relatively small intervention compared to what comes later. Do not wait and watch a brown spot — have it evaluated promptly.

5. Rough, Pitted, or Uneven Enamel Texture
Run your tongue slowly over all your teeth. Healthy enamel should feel smooth and glassy. If you notice a rough patch, a small pit, or an irregular indentation that you don't remember being there before, that change in texture deserves attention as a potential early sign of tooth decay.
As enamel breaks down, its surface integrity changes. The crystalline structure weakens and the smooth surface becomes irregular. What you are feeling with your tongue is actual structural loss of enamel. Pits in the grooves of molars are particularly common because those areas trap food and bacteria and are harder to clean thoroughly with a standard toothbrush.
Texture changes can sometimes be addressed with dental sealants if caught early enough — a thin protective coating bonded to the tooth surface that prevents bacteria from reaching the grooves. Once a pit has become a true cavity, a filling is necessary. Either way, noticing it early is a significant advantage.
6. Food Consistently Getting Trapped in One Spot
Everyone gets food stuck between teeth occasionally. But if the same spot traps food every single time you eat — especially if floss catches or shreds at that location — this is a meaningful cavity warning sign that should not be rationalized away.
Early cavities create small depressions or rough edges in the tooth surface that act like hooks for food particles. Floss catching or tearing can indicate either a rough cavity edge or an early interproximal cavity (one forming between two teeth) that is not yet visible to the naked eye. These between-the-teeth cavities are some of the most commonly missed by patients because they can't be seen in the mirror.
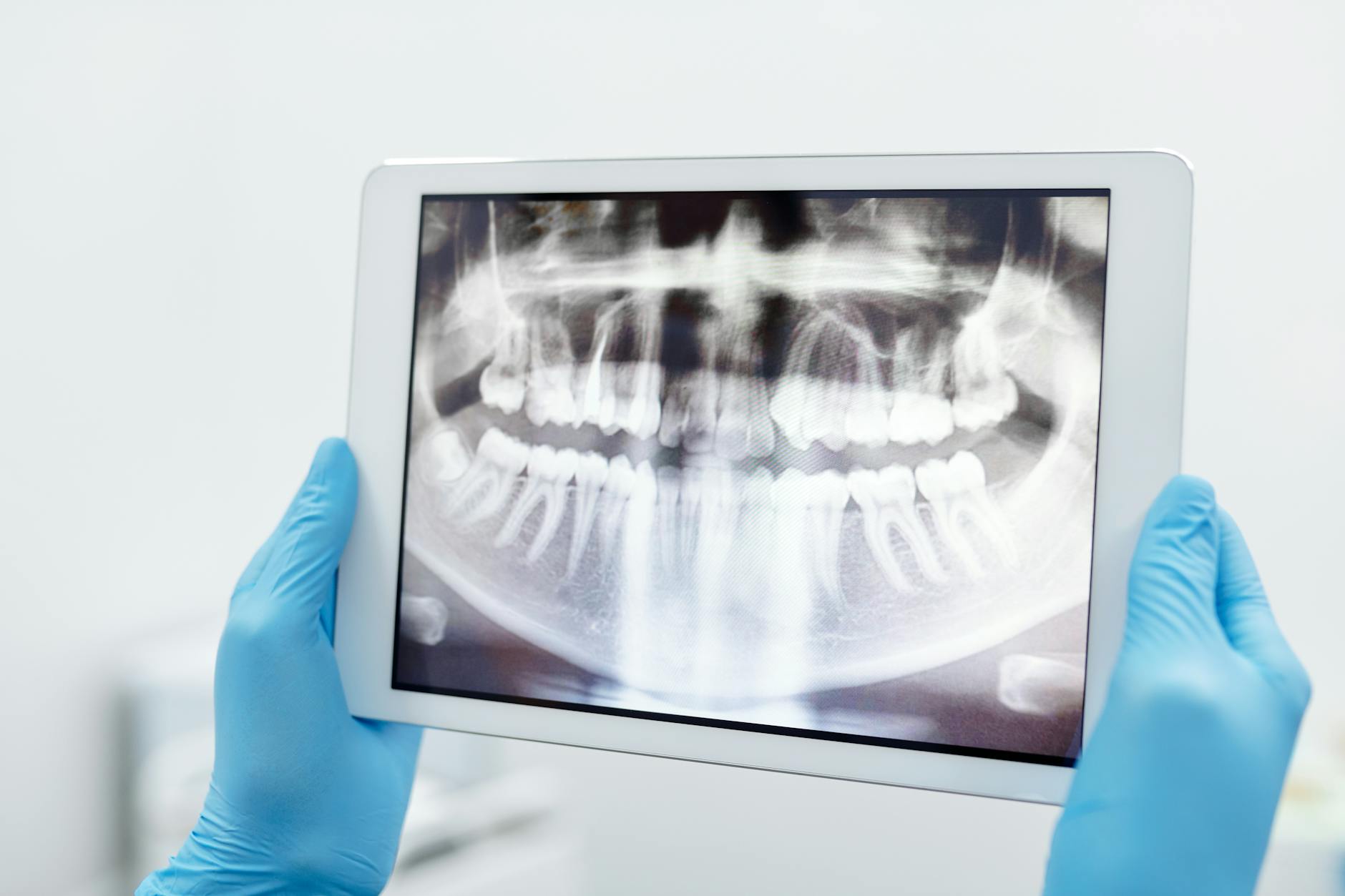
This is precisely why dental X-rays matter: they reveal cavities forming between teeth that only show up on bitewing X-rays. If you have a consistent food-trapping spot, tell your dentist exactly where it is at your next visit. They will target that area specifically during examination.
7. A Visible Hole or Dark Pit in the Tooth
At this stage, there is no ambiguity. A visible hole, dark pit, or crater in a tooth is an unmistakable sign that tooth decay has progressed through the enamel layer and into the dentin beneath. This is a definitive cavity that requires professional treatment — it will not heal on its own.
While this sign may seem obvious, many people postpone acting on it because there is currently no pain. This is a critical mistake. Dentin is softer than enamel and decay spreads more rapidly through it. What looks like a small hole on the surface may already have a much larger lesion beneath it. The window between "visible hole with no pain" and "visible hole with significant pain" can be short.
A filling at this stage is standard and straightforward. Do not delay. The longer a cavity sits untreated, the deeper it progresses toward the pulp, and the more complex and expensive the required treatment becomes.
8. Pain When Biting or Chewing
Pain or sharp discomfort when you bite down is a sign that the structural integrity of the tooth has been compromised. It can indicate either a cavity that has progressed deep into the dentin, a cracked tooth, or both — since decay can weaken a tooth to the point where stress fractures form under the pressures of chewing.
Biting pain is a significant escalation from sensitivity. Sensitivity is a passive response (temperature or sweetness triggers it without physical force). Biting pain means the tooth is responding to mechanical stress, which signals a more advanced structural problem. In some cases, the dentinal tubules under pressure are stimulating the nerve; in others, a fracture is opening slightly under load and compressing pulp tissue.
This symptom should prompt a dental appointment within a few days, not weeks. If you are unable to chew comfortably on one side, the decay or damage has reached a stage where waiting significantly increases risk of more extensive damage.
9. A Constant, Dull, or Throbbing Ache
A toothache that does not go away — a persistent dull throb or ache that may radiate into the jaw or ear — is one of the most serious cavity warning signs on this list. It strongly suggests that bacteria have reached or are very close to reaching the dental pulp: the inner chamber of the tooth containing nerves and blood vessels.
When the pulp becomes inflamed (a condition called pulpitis), it produces a continuous aching sensation. Reversible pulpitis can sometimes be resolved by treating the cavity and removing the source of irritation. Irreversible pulpitis — where the pulp has been too severely damaged — typically requires a root canal to remove the infected tissue and save the tooth.
Do not take painkillers and wait on a persistent toothache. While pain management while waiting for an appointment is reasonable, using it to defer the appointment is not. A throbbing ache signals that a relatively simple filling is no longer sufficient — the longer you wait, the higher the chance the tooth cannot be saved at all.
10. Sharp, Spontaneous Pain — Including at Night
Sharp, shooting pain that occurs with no obvious trigger — or that wakes you from sleep — is the most urgent signal on this list. Spontaneous pain that arises without hot, cold, sweet, or physical provocation indicates that the nerve inside the tooth is severely inflamed or that an abscess (a pocket of infection) has formed at the root tip.
A dental abscess is a serious infection. Left untreated, it can spread to surrounding bone and soft tissue. In rare but documented cases, untreated dental abscesses have led to life-threatening systemic infections. Additional warning signs of an abscess include facial swelling, a pimple-like bump on the gum, fever, and a bad taste in the mouth.
If you are experiencing spontaneous severe tooth pain alongside facial swelling or fever, seek emergency dental care or go to an emergency room immediately. This is no longer a "wait for next available appointment" situation. This is a medical emergency.
What to Do When You Notice These Warning Signs
The most important action for any of the above signs is to schedule a dental appointment — and not to talk yourself out of it. Many people delay because of cost, anxiety, or hope that the problem will resolve itself. Tooth decay does not resolve itself. It progresses. Every week you wait is a week that bacteria are doing more damage.
Here is what treatment looks like at each stage:
- Signs 1–3 (white spots, early temperature/sweet sensitivity): Remineralization therapy. Prescription-strength fluoride varnish, hydroxyapatite treatments, or professional fluoride application can reverse early lesions. No drilling required.
- Signs 4–5 (discoloration, rough texture, early pitting): Dental sealants for at-risk grooves; small composite fillings where enamel has broken down. Quick, affordable, and predictably effective.
- Signs 6–7 (food trapping, visible hole): Composite or amalgam filling. The tooth is numbed, decay is removed, and the cavity is sealed. One appointment in most cases.
- Signs 8–9 (biting pain, persistent ache): Possibly a larger filling, inlay/onlay, or crown if the tooth's structural integrity is compromised. May require root canal therapy if pulp involvement is confirmed.
- Sign 10 (spontaneous pain, swelling, fever): Emergency care. Root canal or extraction depending on the tooth's condition. Antibiotics for infection. Immediate professional evaluation required.
While you wait for your appointment: avoid temperature extremes on the affected side, use a toothpaste formulated for sensitive teeth to help manage discomfort, rinse with warm salt water to reduce bacterial load, and avoid sugary foods and drinks that will fuel further acid attacks on the damaged area.
How to Prevent Tooth Decay Before It Starts
Understanding the early signs of tooth decay is powerful, but prevention is even more so. The good news is that the biology of decay is well understood, and the preventive strategies are simple, inexpensive, and highly effective when applied consistently.
Brushing technique matters as much as frequency. Brush twice daily for a full two minutes using a soft-bristled toothbrush and fluoride toothpaste. Use gentle circular motions rather than aggressive horizontal scrubbing, which can wear enamel and damage the gumline over time. Pay special attention to the gumline and the backs of your molars — these are the areas most likely to develop cavities.
Floss every single day. No amount of brushing cleans the contact points between teeth — only floss does. Interproximal cavities (those forming between teeth) account for a significant proportion of all cavities, and they are entirely preventable with daily flossing. If traditional floss is difficult to manage, floss picks or a water flosser work equally well.
Reduce frequency of sugar exposure, not just quantity. Every time you eat or drink something sugary or acidic, your mouth enters an approximately 20-minute acid attack cycle. Sipping sugary drinks throughout the day is far more damaging than drinking the same amount in one sitting. Limit snacking between meals, and rinse your mouth with water after eating.
Support your saliva. Saliva is your mouth's natural defense against decay — it neutralizes acids, delivers remineralizing minerals, and clears food debris. Stay well hydrated, chew sugar-free gum containing xylitol after meals to stimulate saliva flow, and speak to a doctor if you experience chronic dry mouth, which significantly raises your decay risk.
Consider remineralizing products. Toothpastes and mouthrinses containing fluoride or nano-hydroxyapatite have been shown to actively repair early-stage enamel lesions. These are particularly useful if you are prone to cavities or have been told you have soft teeth.
Don't skip dental checkups. Even with perfect home care, professional cleanings remove calculus buildup that a toothbrush cannot address, and dental X-rays catch interproximal cavities before they become visible or symptomatic. A twice-yearly cleaning and exam is the single most cost-effective investment you can make in your dental health.
Key Takeaways
Tooth decay is a slow, predictable process — and that is actually good news. It means there are multiple opportunities to catch it and intervene before it becomes painful, expensive, or irreversible. The early signs of tooth decay tell a clear story if you know how to read them: from chalky white spots and mild sensitivity all the way to spontaneous pain and swelling.
The earlier you act, the simpler the solution. A white spot can be reversed with no drilling at all. A small cavity takes one short appointment. A neglected abscess can require emergency surgery. The difference between those outcomes is often just a matter of recognizing the warning signs and responding promptly.
If anything in this article sounded familiar — a spot you've been watching, a twinge you've been ignoring — take that as your signal. Book the appointment. Your future self will be grateful you did.
The bottom line: Tooth decay caught at stage 1 or 2 requires no drilling and costs a fraction of later-stage treatment. Knowing the 10 warning signs — from white spots and temperature sensitivity to persistent aches and spontaneous pain — gives you the knowledge to act early, protect your teeth, and avoid unnecessary pain and expense.